Breathe Easy: Advanced Care at our Department of Respiratory Medicine
Breathing is something most of us take for granted. We inhale and exhale approximately 22,000 times a day without a second thought. But for those living with chronic respiratory conditions like Asthma or COPD (Chronic Obstructive Pulmonary Disease), every breath can feel like a victory. In Kenya, where air quality and urbanization are changing our environment, the need for specialized lung care has never been greater.
At LifeCare Hospitals Kenya, our **Department of Respiratory Medicine** is dedicated to diagnosing, treating, and managing conditions that affect the lungs and bronchial tubes. We combine state-of-the-art diagnostic technology with a patient-centered approach to help you reclaim your lung capacity. in this blog, we take a deep dive into how we treat two of the most common respiratory challenges: Asthma and COPD.
1. Understanding Asthma: The Reactive Lung
Asthma is a chronic condition where your airways narrow and swell and may
produce extra mucus. This can make breathing difficult and trigger
coughing, a whistling sound (wheezing) when you breathe out, and
shortness of breath.
Key features of our Asthma care:
- Trigger Identification: We help you identify what sets off your attacks—be it dust, pets, cold air, or exercise.
- Step-Up/Step-Down Therapy: Our pulmonologists adjust your medication levels (preventers and relievers) to ensure you are on the lowest effective dose.
- Inhaler Education: Many asthma treatments fail simply because of poor inhaler technique. We provide hands-on training for all patients.
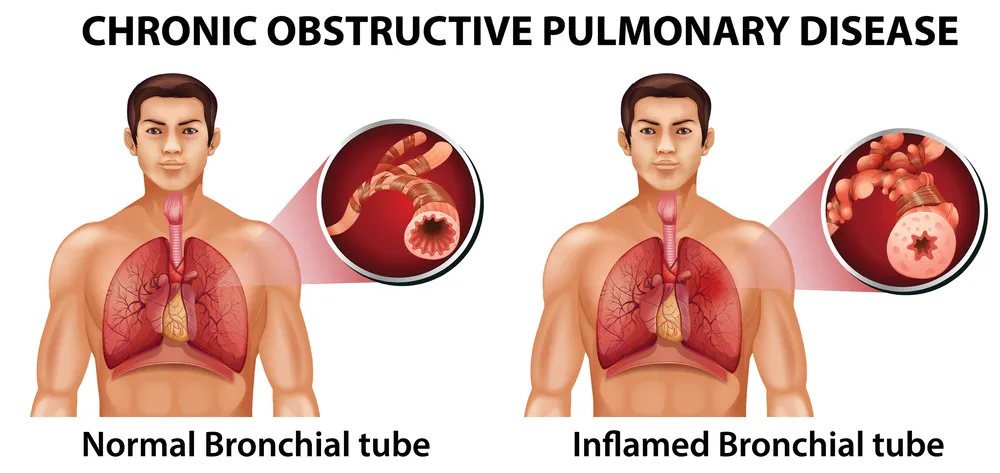
2. COPD: The Progressive Challenge
COPD is a chronic inflammatory lung disease that causes obstructed
airflow from the lungs. Symptoms include breathing difficulty, cough,
mucus (sputum) production, and wheezing. It is most often caused by
long-term exposure to irritating gases or particulate matter, most
commonly from cigarette smoke or indoor cooking fires.
While COPD is progressive (meaning it gets worse over time), it is
highly treatable. With proper management, most people with COPD can
achieve good symptom control and reduced risk of other associated
conditions.
3. Diagnostic Excellence at LifeCare
You cannot treat what you haven't accurately diagnosed. Our department is equipped with:
- Spirometry: The gold standard test that measures how much air you can inhale and exhale, and how fast you can exhale.
- Peak Flow Monitoring: Portable devices to help patients monitor their lung function at home.
- Digital Chest X-Rays & CT Scans: To rule out other conditions like pneumonia, lung scarring, or tuberculosis.
- Arterial Blood Gas (ABG) Analysis: To measure the levels of oxygen and carbon dioxide in your blood, providing a clear picture of how well your lungs are functioning.
4. Comprehensive Treatment Strategies
We don't believe in just "giving a prescription." Our treatment plans are multi-faceted:
- Bronchodilators: Medications that relax the muscles around your airways to make breathing easier.
- Inhaled Steroids: To reduce the underlying inflammation that causes airway swelling.
- Pulmonary Rehabilitation: A specialized program of exercise and education to help you regain stamina and improve your breathing efficiency.
- Oxygen Therapy: For advanced COPD patients who require supplemental oxygen to maintain healthy organ function.
5. Managing Exacerbations (Attacks)
A respiratory crisis—where you suddenly cannot breathe—is a medical emergency. LifeCare Hospitals provide 24/7 care for acute respiratory distress. Our ICUs are equipped with advanced ventilators and our staff is trained in rapid-response respiratory therapy. If you are struggling to breathe, do not wait; visit our emergency room immediately.
6. Lifestyle and Lung Health
Good respiratory medicine includes helping you change your environment:
- Smoking Cessation: We provide support and counseling to help you quit for good.
- Vaccination: We strongly recommend annual flu shots and pneumococcal vaccines for all our chronic respiratory patients to prevent life-threatening complications.
- Internal Monitoring: Regular check-ups even when you are "feeling fine" to adjust treatment before a crisis occurs.
Conclusion: Reclaiming Your Quality of Life
Asthma and COPD change the way you interact with the world, but they don't have to stop you. With the expert guidance of the respiratory team at LifeCare Hospitals Kenya, you can learn to manage your symptoms, increase your activity levels, and breathe with confidence again.
If you have a persistent cough, chronic wheezing, or find yourself getting "winded" easily, it's time to check your lungs. Visit the Department of Respiratory Medicine at LifeCare today. We have the expertise, the technology, and the compassion to help you breathe a sigh of relief. Your lungs are your life—let’s take care of them together.
Frequently Asked Questions (FAQs)
Can kids outgrow asthma?
Many children do see a significant reduction in symptoms as they reach adolescence and their airways grow larger. However, the underlying tendency for "reactive airways" often remains, and asthma can resurface later in life due to environmental triggers or smoking.
What is the difference between asthma and COPD?
Asthma is often triggered by allergies and the narrowing of airways is usually **reversible** with medication. COPD is a permanent, progressive damage to the lung tissue and is usually the result of long-term exposure to smoke or pollutants. However, some patients have an "overlap" of both conditions.
Does using a nebulizer at home replace a hospital visit?
**No.** A home nebulizer is for managing mild to moderate symptoms. If you find that the nebulizer is not providing relief, or if your fingernails or lips are turning blue, it is a life-threatening emergency that requires immediate hospital intervention.
Can diet affect my breathing?
**Yes.** Being overweight puts pressure on your diaphragm and lungs, making breathing harder. Some patients also find that high-sodium diets lead to fluid retention, which can aggravate heart and lung issues. A lean, anti-inflammatory diet overall supports lung function.
